Support Hidden Compass
Our articles are crafted by humans (not generative AI). Support Team Human with a contribution!
Sitara Siverls is sitting at the bedside of a bald Caucasian man in a dimly lit intensive care unit (ICU) room, holding his hand. Outside in the hall, doctors and nurses move briskly. Inside the patient’s room, the wall-mounted TV is on, but the volume is turned down. The only sounds are the beeping of the man’s monitor and the sound of his crying.
It’s early 2021, and the man, who is in his 60s, has COVID-19. He thinks he’s going to die, but Sitara — a 35-year-old trauma ICU nurse at a hospital in the San Francisco Bay Area — is telling him he’s going to be OK.
“The hard part’s over,” she says. “You just have to make it over this hump, and you’re good.”
But the man doesn’t believe her. He can’t stop crying, and his scared, desperate eyes are locked with hers. She hands him a tissue and keeps trying to reassure him, but her words have little effect.
Sitara looks at the clock and realizes she has to go. She tells the man, but when she starts to pull away, he grabs her hand and squeezes it tightly, begging her not to leave. Sitara explains that she has to care for other patients now. But he won’t let go.
It happens all the time. And it kills her every time. Finally Sitara has to pull her hand away forcefully, stand up, walk out of the room, and leave the patient behind.
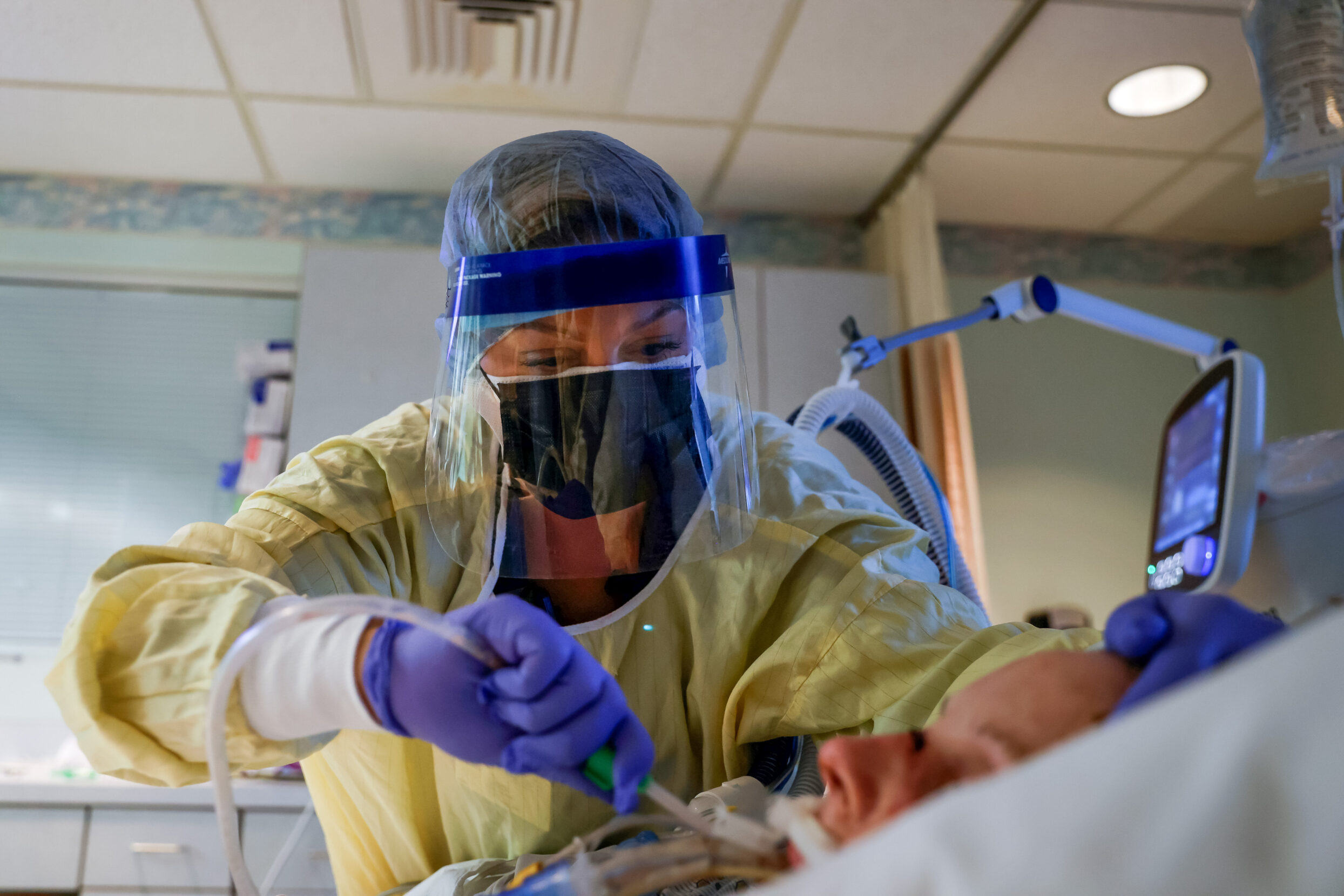
A nurse treats a COVID-19 patient in their isolation room in the ICU. Photo: Shannon Stapleton / Reuters.
~~
Later that year, Sitara is a few hundred miles away from the hospital, lying on a surfboard in the Pacific Ocean. Waves roll under her gently, and the sky overhead is crystal blue. Other people are bobbing around her on surfboards, but she doesn’t pay attention to them. She’s focused on how the ocean feels. The way the waves nudge her this way and that.
Sitara always wanted to try surfing. She lives near a beach, but never found the time — until now.
She’s in Santa Barbara, California, and it’s the first time she’s traveled anywhere alone. A social person, Sitara is usually with friends or her partner when she travels. But this time, out on the water, she’s relishing the solitude. She’s a strong swimmer, so she isn’t scared. And when she doesn’t manage to stand up on the board, she doesn’t care. Just being out in the ocean feels relaxing, peaceful.
The other people near Sitara are fellow nurses and health care workers, plus a few surfing instructors. Like Sitara, the medical professionals are here because they needed a break — the kind provided by an organization called First Descents. Since April 2020, the nonprofit has been taking burnt-out health care workers on outdoor adventure trips — free of charge.

A group from First Descents gathers their kayaks. Photo: Melissa Markle / First Descents.
Some participants, like Sitara, aren’t stereotypical outdoor adventurers who head to the mountains every weekend to go rock climbing or backcountry camping.
But during the pandemic, Sitara started spending more time hiking. She soon realized, as the scientific community has long known, that time in nature was good for her well-being.
Decades of research demonstrate the benefits of being in nature: boosts in cognition and eyesight, reductions in depression and diabetes, improved heart health and immune function. Before the pandemic, First Descents harnessed this transformative power of nature by taking young adults affected by cancer and other serious health conditions on these outdoor adventures.
But when gatherings became too risky for immunocompromised participants, the organization shifted focus, to embrace an unprecedented opportunity. They saw a way to deliver some of the well-researched benefits of time in nature — reduced stress and anxiety, and improved social connectedness and physical health — to the overstressed health care workers on the front lines of the global pandemic.
Sitara signed up as soon as she discovered First Descents.
Getting up on the surfboard is more difficult than Sitara imagined, but exerting her body in the effort feels surprisingly new. She’s not just enlisting a group of muscles. She’s not just pushing through a physical challenge.
She’s digging, deep down, searching for something.

Nurses and other health care workers affected by their time treating COVID patients tackle the waves with First Descents. Photo: Philip Robinson / First Descents.
~~
Until COVID, Sitara loved going to work and felt like she was doing what she was meant to do. Her first introduction to the profession was through her role model, her mom, who is also a nurse. But it was college science classes — microbiology, anatomy, and physiology — that sparked Sitara’s interest in a medical career. She wanted to explore ways to help heal people. In 2014, she became a registered nurse.
Working in the ICU — where patients often go from unconscious to completely alert — brings the challenges and rewards of her profession into sharp focus. When a patient regains consciousness, Sitara can give them “that emotional boost that they need to keep their hope alive and to build their confidence.”
And leaping into action when a patient is crashing — when their heart stops — is a full-on adrenaline rush. “It’s very Hollywood,” Sitara says. “You get the pulse back, and you monitor them closely, and you just pray on it. And then if you are lucky enough to keep that same patient, you can see how they evolve and grow from literally knocking on death’s door to waking up and being taken off a ventilator.”
For years, Sitara thrived as an ICU nurse.
~~
‘I need you to just be positive and hold on.’
At COVID’s peak, in January 2021, more than 700 people died in one day in California.
Sitara’s patient who couldn’t stop crying recovered and was discharged. But other COVID patients were still dying at the hospital, one after another, every single day.
“You think they’re exaggerating what they show on the news — this person’s holding her hand, and she’s dying,” Sitara says. “That’s literally what’s happening, and it’s crazy. It’s depressing.”
When COVID protocols barred hospital room visitors, nurses were often a patient’s only source of comfort.
“They don’t even know me,” Sitara, a Black woman, says. Yet they had no choice but to lean on her — even the white woman who told her she hated Black people. (The woman later apologized. When people are dying, Sitara says, “they respect you for being a person, and they thank you.”)
Sitara often sat with these patients in their last moments, keeping them company as life slipped out of them. Then she would have to move right on to the next patient. There was no time to process her grief.
Drained and overwhelmed by the pandemic’s effect on the hospital, Sitara felt angry that her job — which is hard under any circumstances — had become even harder.
The sadness and frustration of not being able to help patients built up. Sometimes the equipment Sitara was given to do her job seemed inadequate. Sometimes she resented “being the scapegoat [in] a process that you have no control over.” When dealing with patients’ family members, Sitara says she and her colleagues “get yelled at, we get cursed at, we get threatened.”
She started to hate the work she’d once loved.
Some of her colleagues seemed to handle the stress and grief better than she did. And that made her feel even worse, adding guilt to the mix. Why do I hate my job right now and they don’t? Sitara remembers thinking. Or do they hate it too, and just hide it better?
One day, when she walked out the door at the end of a 16-hour shift, she thought to herself, It might be time to quit.
~~
What Sitara didn’t know was that her experience wasn’t unique. COVID pushed health care workers to levels of burnout unprecedented in modern times. A May 2022 Surgeon General’s Advisory warned that since the pandemic began, more than 50% of medical workers in the United States reported symptoms of at least one mental-health condition such as depression or PTSD.
He can’t stop crying, and his scared, desperate eyes are locked with hers.
On one occasion, at a birthday party, Sitara was introduced to a woman who said she wanted to be a nurse.
Sitara looked at her and responded bluntly: “Why?”
~~
Leaning forward into the firelight, Sitara looks around the circle of people and says, “I go to work every day, and I say: What the fuck am I doing?!?”
It’s the end of Sitara’s first day in Santa Barbara. She and her peers are sitting around a fire pit adjacent to their hotel, trading war stories and drawing succor from their shared vocation. She looks around at her fellow health care workers, their faces illuminated by the flickering firelight.

Medical care workers gather around the fire pit to share personal stories of struggle, strife, and renewal during a First Descents retreat. Photo: Melanie Fidler / First Descents.
Most of these dozen or so participants are women and nurses, but there are a few men, a physical therapist, and a doctor too. It’s a pretty diverse bunch: Sitara and a couple of other people are Black; the rest are Asian, Indian, and white. Personality-wise, they run the gamut from chatty and expressive to reticent and introverted.
They don’t know each other’s names. At the beginning of the trip, everyone picked a nickname — kind of like a call sign.
It feels like a safe space to say what’s on her mind. But Sitara’s not used to this kind of open conversation with these kinds of peers. As the words leave her mouth, she’s not sure how the others will react.
When a couple of them immediately throw their heads back and laugh, she’s relieved. A few more look right at her and nod knowingly.
One by one, her peers share what they’ve been dealing with, releasing their pent-up sadness, frustration, and anger. Sitara looks at each of them, hears them, and thinks, These people understand. They get it.
Since the pandemic began, more than 50% of medical workers in the United States reported symptoms of at least one mental-health condition such as depression or PTSD.
She’s only been away from home for 24 hours, but sitting now in front of a cozy, crackling fire, surrounded by people who know her daily challenges firsthand, she already feels different. More grounded.
A firepit next to a hotel isn’t exactly what Sitara was expecting for this session. She’d envisioned something more secluded and nestled in nature, maybe surrounded by trees. But the fire, like the group itself, is warm and inviting.
The weight Sitara has been carrying around is familiar to every one of these people. Every one of them knows what it’s like to be a front-line worker during a pandemic. Every one showed up in Santa Barbara with some version of trauma or PTSD. Though Sitara’s friends and family are supportive, she feels that only the people who do what she does can really, truly, get it.
Sitara identifies most directly with the nurses in the group. But she appreciates the perspective of the doctor, who shares the personal guilt he feels as the person in charge of each patient’s plan of care. While nurses often grieve because they sit at the bedside of people dying, Sitara realized that doctors like this man often grieve because they think about what they could have done differently.
It helps that Sitara probably won’t see any of these people again. She won’t have to relive her shame if someone reacts badly to something she says.
But that’s not what’s happening. Everyone is supportive. There’s no judgment. As the night wears on, the mood goes from light to somber and back again. Sitara sees anger, pain, and laughter play across her peers’ faces. The same as they play across hers.
Later, when the session is over, several people thank Sitara for saying what she said. Because that’s exactly how they feel too.
Sitara has always appreciated the public efforts so many people have made to honor and support her profession during the pandemic. But some of the things she’s seen — “Health Care Heroes” signs, for instance — ring a little hollow. They don’t help.
This, she thinks, as she gets up from the fire pit and heads to her hotel room, is the only thing that has.
~~
The National Institutes of Health (NIH) is in its second year of studying the effects of First Descents’ programs — whether and how they reduce stress and increase resilience and wellbeing in health care providers. Researchers are measuring the impact on the anxiety, depression, stress, post-traumatic stress, sleep quality, and burnout of 90 health care workers.
The NIH’s study is ongoing, so findings aren’t available yet. But First Descents collects its own quantitative and qualitative data on the effects of its programs, which have served more than 689 health care workers across the U.S. so far. Mackenzie McGrath, First Descents’ vice president of programs, shares that according to their data 94% of participants report increased hopefulness and positivity after a nature trip, 89% have increased self-confidence, and 87% feel less depressed and anxious.

A First Descents kayaker embraces a moment of elation. Photo: Regina Nicolardi / First Descents.
“We do know that nature heals, and time outside — just 15 minutes alone — has mental health benefits,” McGrath says. “So there’s science behind that.”
Of course, cures for health care burnout are crucial, but they shouldn’t obscure the necessity of prevention. If the health care system could avoid worker burnout in the first place, radical post-burnout interventions — like First Descents nature trips — would be unnecessary.
Still, says McGrath, addressing an existing problem before it gets worse is sometimes the best you can do.
~~
Sitara is clutching the sides of her surfboard, trying hard to get on top of it. She can’t believe how much upper-body strength it requires.
She digs inside again, then pushes out. As hard as she possibly can. It feels like she’s releasing something. Like she’s physically pushing out what she doesn’t want or need — her pent-up stress and grief and sadness and pain.
She’s also learning to let go of what she can’t control. Being in nature, she says, “makes you realize the world is a lot bigger than your own problem.” Even if she learns to master the surfboard, she’ll never be able to control the waves.
There’s only one thing to do with waves, she realizes, whether in the ocean or in her life: “You go with them.”

A surfer relaxes in calm waters off the coast of southern California. Photo: RooM the Agency / Alamy.
~~
During the height of the pandemic — before she paddled into the Pacific Ocean with First Descents — Sitara stood over a COVID patient named Stephanie, checking the monitor next to her bed. Stephanie, who was in her 50s or 60s but looked like she was in her 40s, was unconscious and hooked up to a ventilator.
A man’s voice filled the room, reciting a verse from the Bible. But Stephanie’s husband wasn’t there with them. His voice was coming from a small recorder on the table next to her bed.
The man himself was standing just outside the room, in the hallway facing Stephanie, with his arms held up in the air and his eyes closed, praying. The glass door blocked the sound, so his wife wouldn’t have been able to hear him there, even if she were conscious. That’s why he started making recordings of his voice, which Sitara played for Stephanie every shift.
Many of the recordings were of Stephanie’s husband quoting scripture. But sometimes he said other things, like when he’d tell his wife how much he loved her and how much hope he had for her. “He’d say, ‘Stay strong, stay strong,’” Sitara says.
And sometimes the recordings consisted of hours-long interviews with Stephanie’s friends and family, so that she could hear their voices too.
Sitara doesn’t remember the husband’s name, but she remembers Stephanie’s — in part because Sitara intubated her. “I remember having these conversations with her, her being scared, me giving the pep talk that I give everyone,” Sitara says. “I remember saying to her, [‘You’re] going to be OK, we’re doing this [intubation] early, it’s just going to be temporary. I need you to just be positive and hold on.’”
Stephanie’s husband visited her nearly every day, and called to check on her often. Sitara remembers worrying that he needed to take a break, so she spoke to him about caregiver stress, but she admired his devotion to his wife.
One day, after Sitara had been off for a few days, she came back to work to learn Stephanie had died. Another nurse had provided Stephanie’s comfort care at the end of her life.
Sitara still deals with oceans of sadness for Stephanie and the many, many other patients Sitara has lost — not to mention their grief-stricken families. And then there’s still the myriad daily stresses of a shift in the ICU ward.
Even if she learns to master the surfboard, she’ll never be able to control the waves.
But thanks to her First Descents trip, Sitara says she’s getting better at dealing with all of that. After she saw how others in her Santa Barbara group created a separation between their jobs and personal lives, she changed her work schedule so she has several days off in a row. She always plans something she can look forward to, like hiking and kayaking.
Sitara has also become better at letting go of her anger and sadness and all the things she can’t control. She’s decided “to accept my role as being a nurse and being the best person that I can be within that role, so I can make a difference to whomever I work with and who I touch.”
Stephanie’s hospital stay happened before Sitara took to her surfboard in Santa Barbara. But her memories of Stephanie and her husband point to ways she has managed to make a difference — even in the hardest moments of a pandemic.
~~
After Stephanie’s passing, her husband called one more time — to thank Sitara and her colleagues. He came to the hospital with a personalized package for each of them. Inside was the program from Stephanie’s funeral, a CD of the service, her obituary, and a little religious pamphlet he’d made.
Sitara’s voice still cracks when she talks about the man. No one else has ever done anything like that to thank her.
Now Sitara always tells family members that if they make a recording, she’ll play it in the patient’s room. She asks what kind of music the patient likes, so she can put it on even if they’re unconscious. It’s a small thing she can do to bring them some comfort — which is a big part of what drew Sitara to nursing in the first place. It’s why, despite everything, she still loves being a nurse.
“I want people to heal,” she says, “in any way that I can allow that to be.”
Allison Torres Burtka
Allison Torres Burtka is a freelance writer and editor who loves to write about the transformative power of sports and the outdoors.



